A Search for Unexpected Genetic Heroes
for Mount Sinai
Problem
A paper-based consent process is cumbersome, requires enormous human effort from the clinical staff to patients to fill out, doesn’t scale, can’t be transferred or reused, and the process is most often abandoned leaving all parties in the lurch.
Solution
We designed a service that would allow patients to digitally decide if they want to participate in research studies or release their data to R&D organizations to allow clinicians to test and report on it. A cloud-based, open source, SaaS (software as a service) framework would allow any hospital to transition from the current clumsy paper-based process to a hyper-personalized, analytics-driven consent process.
Results
The project was unveiled at TED with the presentation of a result report for The Resilience Project and has helped to collect over 600,000 individuals.
Time: 1 designer for 3 months
Tags: Precision Medicine and Genomics
Process
Eric Schadt1, director of the Icahn Institute for Genomics and Multiscale Biology at Mount Sinai Hospital, and Elissa Levin2, assistant professor of Genetics and Genomic Sciences at Mount Sinai, tasked GoInvo to develop a smooth electronic consent platform for patients to participate in genomics studies. With consent as a highly regulated space and blessing from Mount Sinai Hospital’s IRB (institutional review board), open source eConsent would be a global coup for clinical research.
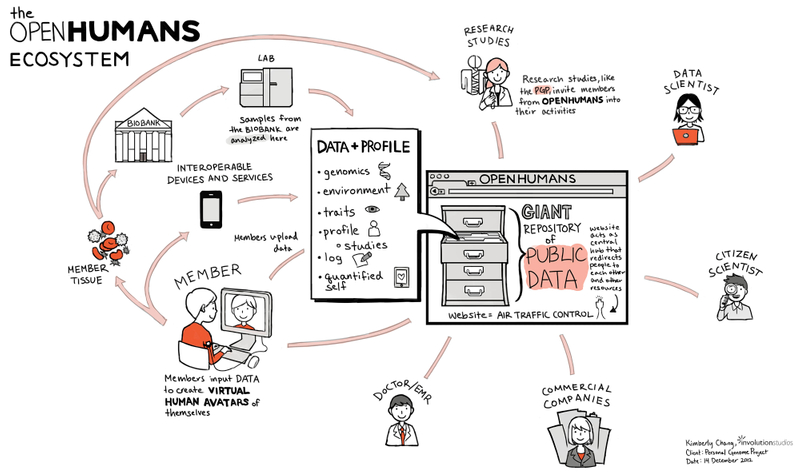
We began by mapping out the ecosystem around eConsent, using genomics testing as a baseline. At Mount Sinai Hospital, genomics testing frequently occurs during the IVF process (in vitro fertilization). Not so coincidentally, Dr. Alan Copperman3 runs one of the busiest and most progressive IVF clinics4 in mid-town Manhattan. He was our early adopter, our clinical feedback loop, and educator.
Experiencing the pain first hand
To better understand IVF, we made an appointment with the mid-town clinic as parents wanting to have a child through IVF. We went through the preliminary process and training at RMA NY.

The required paperwork, clinical scheduling, diet, and fertility drugs routines were staggeringly complex and painful to implement (from our discussions with current and past patients). Almost half of couples don’t make it beyond the initial training seminar and paper-based consent. The IVF clinic nurses and administrators yearned for a digital consent service accessible from patients’ phones, tablets, and desktops to track them through the process, drive up completion and efficiency rates, and ultimately provide a better experience with IVF.
Creating a strong solution
Genetics for Non-Geneticists and simplicity in a complex system
Elissa Levin, was the driving force for delivering a working eConsent service for The Resilience Project. As a former genetic counselor, she knew the difficulty in describing the complex lab results to doctors and patients. Those very personal results need to be easily digestible by patients, proxies, and doctors (because many docs aren't up on genomics).
Genomics is brutally complicated. Patients struggle. Doctors flounder. Invo made them all smile.
Elissa Levin
Head, Genomics and Integrative Health Innovations, Icahn School of Medicine at Mount Sinai
Doctors and administrators have near zero insight into what patients have consented to (it's mostly faxed), and patients don't know what consents they've already signed, where their data is, and how it's being used. Imagine having control of your data like the temperature in your house, a Nest for your health data. A patient can proxy Mount Sinai and Mass General Hospital to have their data for the next year, retract data from research studies they’re involved in, and see how their data has impacted someone's health, all while their primary care doctor has read and write privileges as long as the patient is under their care.

Early draft of genetic reporting for couples going through the IVF process.

Genetic experts marking up printed comps with their feedback.
We took a systems approach to designing the consent experience, using what we learned from the initial introduction to IVF, training materials, spit kit, and reporting. We strove towards shepherding want-to-be parents through the long and tiresome process, employing just-in-time training for patients depending on their needs and frustrations (based on analytics and IVF clinic stats), etc.
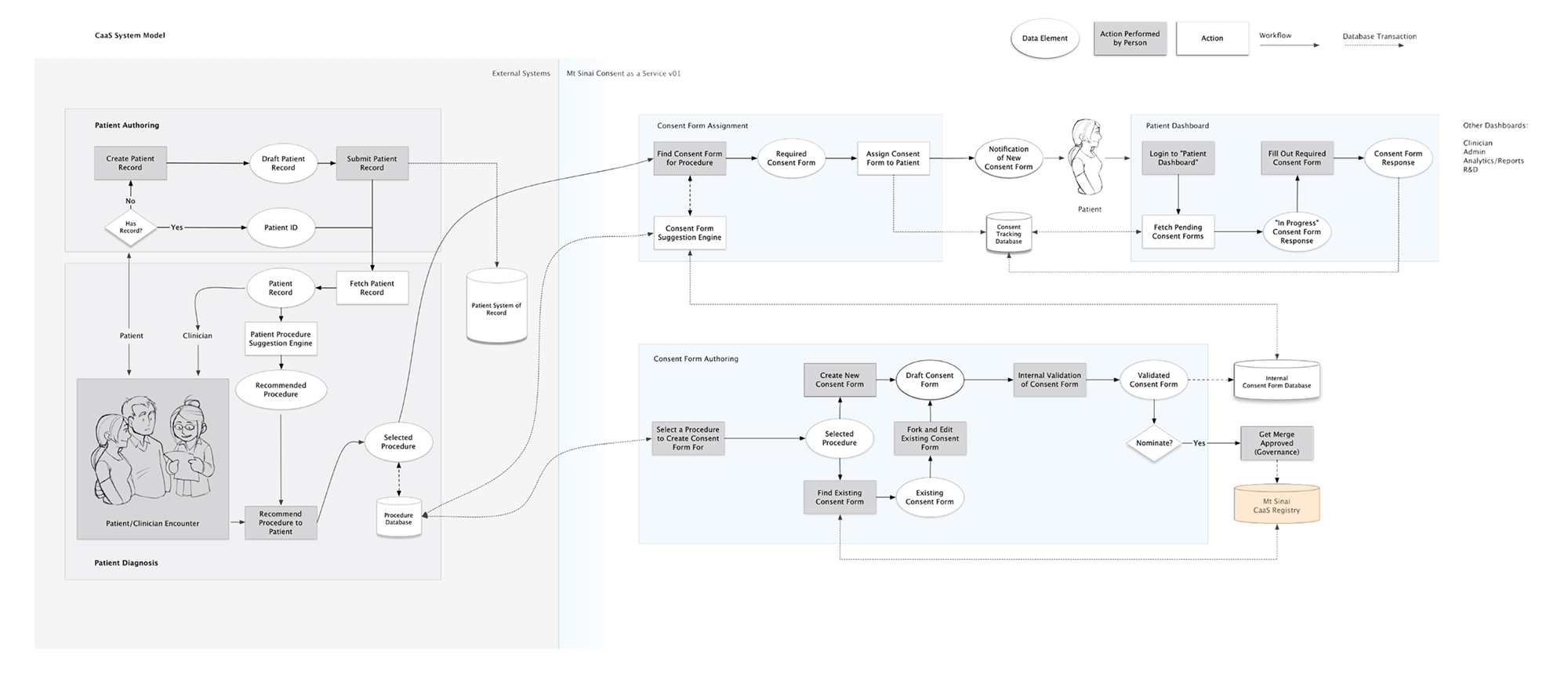
System model of the CaaS (consent as a service) software.
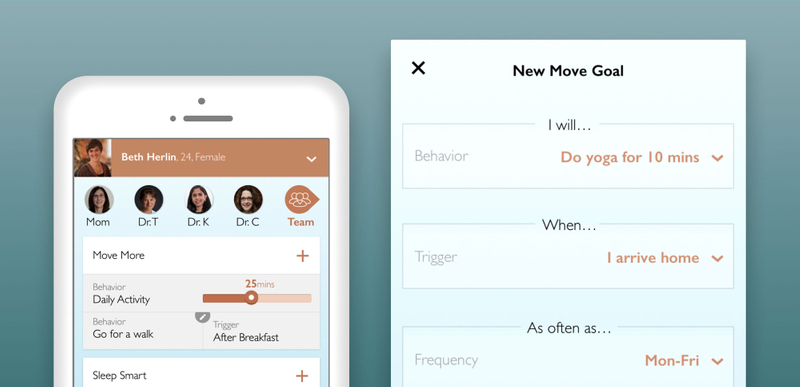
A Push for Mobile Consent
John Halamka, Beth Israel Deaconess Medical Center (BIDMC) CIO and Meaningful Use co-author, proclaimed, "the laptop is dead, the desktop is gone.5” This rings most true for patients, where 77% of adults in the US have smartphones6 in their pockets and likely much higher for IVF patients. Thus it was critical for the patient-facing e-consent to be a mobile service. It also needed to accommodate interactive educational lessons with different learning styles and adaptive content based on the patient's understanding and emotional response. We included a voice user interface (VUI) for listening to and answering questions (vs long-form reading) as well as voice signature capabilities (since digital voice signatures, a form of biometric signatures, offer stronger authentication than hand-written signatures: A Comparison of Digital and Handwritten Signatures7, Biometrics Wiki8). The service also included expression comprehension, captured non-invasively via your phone's camera, to detect in near-real time how a patient was or was not consuming the lesson. The service would adjust content based on the emotional and heart rate response to better match the material and understanding level. Pretty rad, eh?
It was a big hit here at TED!
Elissa Levin
Head, Genomics and Integrative Health Innovations, Icahn School of Medicine at Mount Sinai
Trial Run at TED
The CaaS (consent as a service) project dovetailed with Mount Sinai and Sage Bionetwork's The Resilience Project9, an initiative to sequence 1,000,000 entire human genomes for finding the rare people whom genetically show a condition, such as cystic fibrosis, but exhibit none of the physical attributes.
The mobile e-consent software would be the driving force in getting willing participants to sign up and allow their genomic data to be used for research. Stephen Friend10, a co-Principal Investigator on The Resilience Project, took to the main TED stage and showcased the hunt for unexpected heroes11.
Outside the auditorium, Elissa and other Mount Sinai genomicists collected samples and dished out results, using our report designs.
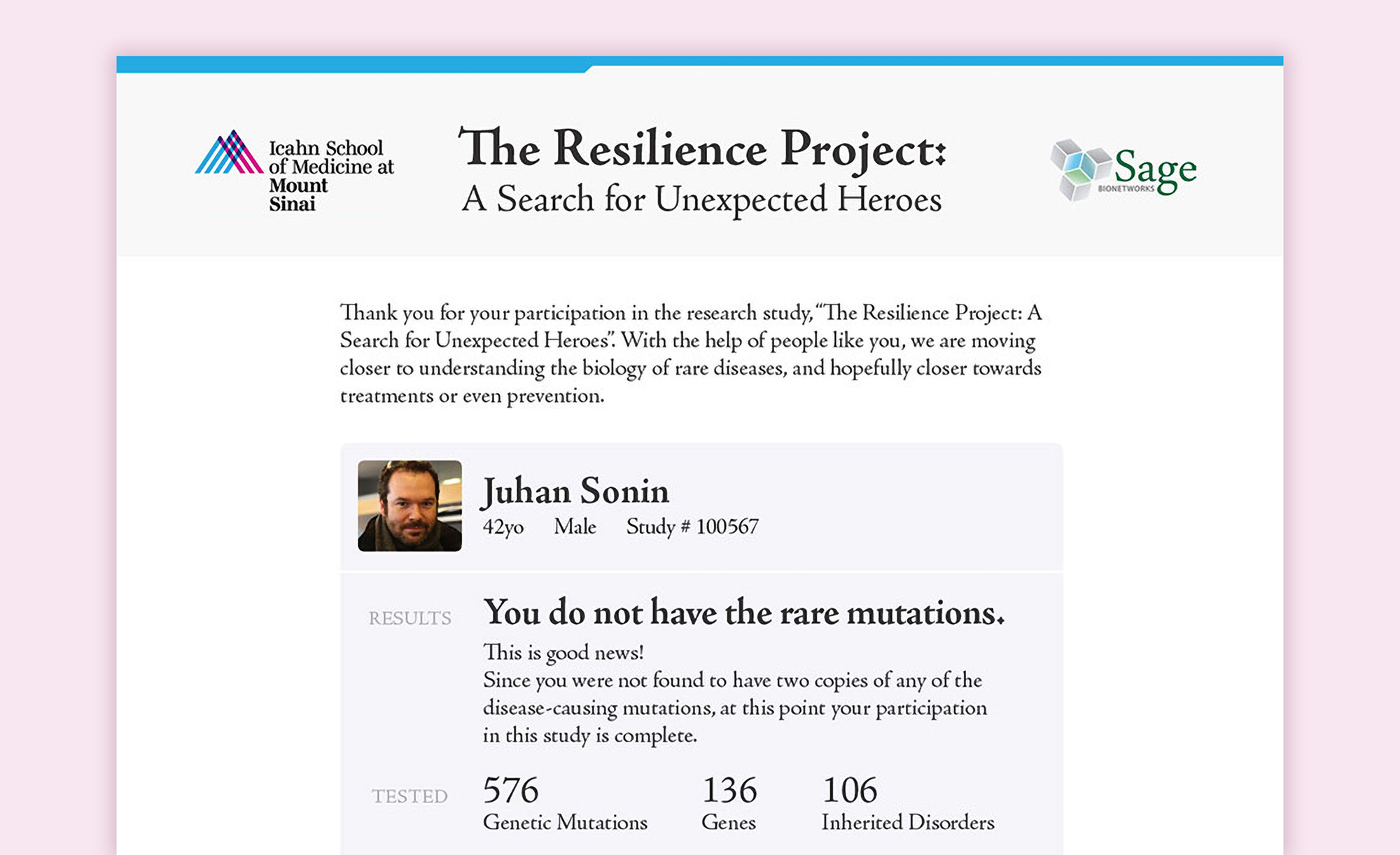
Sample genetic report for The Resilience Project.

Electronic consent workflow for The Resilience Project.
Path Paved for Better Patient Consenting
The success and scale of The Resilience Project hinged on electronic consent. The Mount Sinai team, together with GoInvo, saw a solution to bypass the crazy, analog, and impossible-to-distribute consent process and ultimately give patients an easy-to-understand report on their genetic traits and how their genes could impact their potential offspring.
Up next
References
- About Eric Schadt: http://en.wikipedia.org/wiki/Eric_Schadt
- : https://www.linkedin.com/pub/elissa-levin/4/888/aa
- : https://www.rmany.com/our-team/physicians/dr-alan-copperman
- : https://www.nytimes.com/2014/02/26/health/fda-meeting-considers-controversial-fertility-procedure.html?_r=0
- : http://www.washingtonpost.com/business/on-it/at-one-hospital-iphones-ipads-and-google-glass-become-key-medical-tools/2014/07/13/ce2657b0-0842-11e4-a0dd-f2b22a257353_story.html
- : http://www.pewinternet.org/fact-sheet/mobile/
- : http://groups.csail.mit.edu/mac/classes/6.805/student-papers/fall97-papers/fillingham-sig.html
- : http://en.wikipedia.org/wiki/Biometrics
- : http://www.resilienceproject.me/
- : https://en.wikipedia.org/wiki/Stephen_Friend
- : http://www.ted.com/talks/2004